Telehealth counseling is often framed as “therapy over video.” That description is incomplete. The real transformation is structural. Telehealth is changing who gets access to care, how therapy is delivered, how outcomes are measured, how clinicians practice, and how mental health is financed.
It offers a flexible, accessible alternative to in-person visits, allowing patients to receive professional support for conditions like anxiety, depression, and PTSD from their own homes. Platforms such as Teladoc Health, BetterHelp, Talkspace, and health systems like Mayo Clinic have accelerated adoption, but the deeper shift is systemic, not platform-specific.
Core Pillars of Transformation
| Pillar | What Is Changing | How Telehealth Drives It | System-Level Impact |
| Access | From local supply to digital networks | Video and remote sessions remove travel barriers | Rural & underserved populations gain specialists |
| Economics | From rent-heavy clinics to platform models | Subscription billing & employer contracts | Flexible payment ecosystems |
| Workforce | From clinic-based work to remote practice | Digital scheduling & remote caseloads | Larger labor pool; burnout risks |
| Measurement | From narrative notes to tracked metrics | Mood logs, symptom dashboards | Data-informed care decisions |
| Prevention | From crisis response to maintenance | Ongoing check-ins, wellness integration | Reduced relapse cycles |
| Regulation | From location rules to tele-policy evolution | Interstate compacts & parity laws | Cross-border complexity |
| Technology | From manual processes to AI-supported systems | Automated intake & scheduling | Efficiency with ethical oversight |
Adoption & Growth Trend
Telehealth usage grew gradually pre-2020, spiked during COVID-19, and stabilized into a hybrid norm.
Authoritative bodies such as World Health Organization and National Institute of Mental Health recognize tele-mental health as a viable strategy to address workforce shortages.
The key shift: telehealth is no longer temporary. It is embedded in mainstream healthcare systems.
Medical Scope: Conditions & Treatment
Telehealth is clinically appropriate for many mental health conditions. Professional bodies such as the American Psychological Association support telepsychology when delivered by licensed professionals in accordance with ethical standards.
| Condition | Telehealth Suitability | Treatment Options |
| Mild Anxiety | High | CBT, mindfulness |
| Moderate Depression | High | CBT, medication |
| PTSD (stable) | Moderate–High | Trauma therapy |
| ADHD | Moderate | Behavioral therapy |
| Acute Crisis | Low alone | Requires in-person/hybrid |
| Psychosis | Low | In-person recommended |
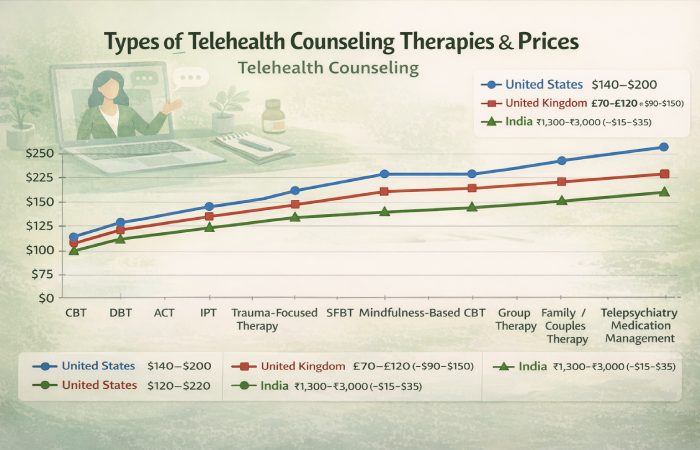
Types of Telehealth Counseling Therapies & Prices
| Therapy Type | Primary Focus | Delivery Format | Best For | Typical Session Length | Approx. Price per Session (USD) |
| Cognitive Behavioral Therapy (CBT) | Changing unhelpful thoughts & behaviors | Video / Phone | Anxiety, depression, phobias | 45–60 mins | US: $100–$200UK: £60–£120 (~$75–$150)India: $10–$35 |
| Dialectical Behavior Therapy (DBT) | Emotion regulation & coping skills | Video / Group | Emotional dysregulation, borderline traits | 50–60 mins | US: $120–$220UK: £70–£140 (~$90–$175)India: $15–$40 |
| Acceptance & Commitment Therapy (ACT) | Mindfulness + values-based change | Video / Phone | Anxiety, chronic pain, depression | 45–60 mins | US: $100–$200UK: £60–£120 (~$75–$150)India: $10–$35 |
| Interpersonal Therapy (IPT) | Relationship & role transition | Video / Phone | Depression, grief, relationship issues | 45–60 mins | US: $100–$200UK: £60–£120 (~$75–$150)India: $10–$35 |
| Trauma-Focused Therapy (TF-CBT, EMDR-adapted) | Processing trauma | Video / Phone | PTSD, trauma histories | 50–90 mins | US: $120–$250UK: £80–£160 (~$105–$200)India: $15–$45 |
| Solution-Focused Brief Therapy (SFBT) | Goal-oriented rapid change | Video / Phone | Specific problem resolution | 30–45 mins | US: $80–$160UK: £50–£100 (~$65–$125)India: $8–$30 |
| Mindfulness-Based CBT (MBCT) | Prevent relapse & stress reduction | Video / Phone | Depression relapse, stress | 45–60 mins | US: $100–$190UK: £60–£120 (~$75–$150)India: $10–$35 |
| Group Therapy (Remote) | Shared therapeutic dynamic | Video | Peer support, social skills | 60–120 mins | US: $40–$100 (group rate)UK: £30–£80 (~$40–$100)India: $5–$20 |
| Family / Couples Therapy | Relational system work | Video | Family conflict, couples issues | 60–90 mins | US: $120–$250UK: £80–£160 (~$105–$200)India: $15–$45 |
| Motivational Interviewing | Behavior change motivation | Video / Phone | Addiction, ambivalence | 30–50 mins | US: $90–$170UK: £55–£110 (~$70–$135)India: $10–$30 |
| Telepsychiatry Medication Management | Psychiatric evaluation & meds | Video | Mood disorders, ADHD | 15–30 mins | US: $150–$300UK: £90–£180 (~$120–$220)India: $15–$45 |
| Digital CBT Modules / Guided Self-Help | Structured self-paced therapeutic exercises | Online / App | Mild depression / anxiety | Self-paced | US: $30–$100/mo (app) UK: £20–£80/mo (~$25–$100)India: ₹300–₹1,500 (~$4–$20) |
Benefits of Telehealth Counseling
| Benefit Category | What It Means | Why It Matters | Who Benefits Most |
| Accessibility | Therapy from home via video/phone | Removes travel barriers | Rural populations, mobility limitations |
| Convenience | Flexible scheduling, evening sessions | Fits around work/school | Working professionals, students |
| Cost Efficiency | Lower overhead = competitive pricing | Reduces total care expense | Self-paying clients |
| Privacy | No waiting room visits | Reduces stigma | First-time therapy users |
| Continuity of Care | Access during travel or relocation | Prevents treatment gaps | Expats, frequent travelers |
| Broader Provider Choice | Access to out-of-city specialists | Better therapist fit | Niche mental health needs |
| Faster Appointments | Shorter wait times | Early intervention | Mild–moderate conditions |
| Integrated Care | Therapy + medication in one platform | Coordinated treatment | Moderate–severe disorders |
| Digital Tools | Mood tracking, reminders, resources | Better progress monitoring | Tech-comfortable users |
| Crisis Triage Support | Immediate tele-screening | Quick risk evaluation | Anxiety or urgent support seekers |
Well-known Doctors in Telehealth & Digital Mental Health
| Doctor / Expert | Primary Specialty | Typical Fee Range for Telehealth Session | Notes / Regional Context |
| John Torous | Psychiatry & Digital Psychiatry Research | $180–$300+ (typical board-certified rate) | Telepsychiatry consults often start ~$200–$300 for initial medication management; follow-ups lower |
| Helen Christensen | Clinical Psychology & Digital Mental Health | $134–$200+ (psychologist range) | Teletherapy consultations with experienced psychologists average $134–$184 per session |
| Vikram Patel | Global Mental Health & Scalable Care | India: ₹800–₹3,450 (~$10–$40) | Indian telehealth psychology and psychiatric sessions typically range from ₹800–₹3,450/session |
| Thomas Insel | Psychiatry Policy & Digital Health Leadership | $180–$400+ (estimated specialist rate) | Senior psychiatrists or consultants often charge above typical telepsychiatry rates due to expertise. |
| Shekhar Saxena | Global Mental Health Policy | $150–$300+ (specialist telepsychiatry) | Policy influencers often consult at specialist telehealth rates. |
| David Gratzer | Telepsychiatry & Healthcare Delivery | $180–$300+ (estimated board level) | Canadian and US telepsychiatry consultations typically sit in this range. |
| Daniel Freeman | Online CBT & Digital Therapy Research | $134–$200+ (psychology consult) | CBT specialists online often charge similar to clinical psychologists. |
| Amit Malik | Telepsychiatry Awareness & Practice | India: ₹800–₹3,450 (~$10–$40) | Tele-mental health pricing in Indian private practice context. |
Telehealth Mental Health Apps & Platforms
| App / Platform | Core Function | Best For | Primary Services | Typical Price Range |
| BetterHelp | Online counseling network | Flexible therapy | Video/phone/messaging therapy | $60–$90/week (subscription) |
| Talkspace | Counselor matching & therapy | Messaging-based support | Messaging + sessions | $65–$90+/week |
| Teladoc Health | Full telemedicine platform | Telepsychiatry + therapy | Psychiatrists + therapists | $85–$300+/session |
| Headway | Therapist matching + insurance | Insurance-backed therapy | CBT, DBT, trauma | Varies by insurance |
| Lyra Health | Employer-provided mental health | Workplace therapy | Screenings, therapy, coaching | Covered by employer |
| Ginger (now part of Headspace Health) | Coaching + therapy + psychiatry | Rapid access support | Coaching + therapy + med management | Employer subscription |
| 1mg / mfine (India) | Doctor consultations including psychiatry | Telepsychiatry in India | Video consults | ₹300–₹1500/session (~$4–$20) |
| Practo | Medical & psychiatric consults | Doctor + therapist access | Video/phone consults | ₹500–₹2500 (~$7–$33) |
| eSanjeevani (India) | Government telemedicine platform | Low-cost psychiatric consults | Video OPD | Free/Subsidized |
| Tele-MANAS (India) | Tele-mental health helpline | Crisis counseling | Phone support | Free |
| Calmerry | Online therapy | Affordable therapy | Chat + video therapy | ~$50–$70/week |
| Amwell | Telehealth + mental health | Therapy + psychiatry | Licensed clinicians | $99–$299/session |
| MDLive (now part of Cigna Telehealth) | Telemedicine + psychiatry | Quick access psychiatry | Psychiatric evaluation | Insurance pricing |
| BetterUp | Coaching-focused | Personal & professional growth | Coaching, not clinical therapy | Employer subscription |
| Talkiatry | Online psychiatric care | Medication management | Psychiatric evaluation + meds | $200–$300 initial |
| MindDoc / Moodpath | Self-monitoring & assessment | Digital screening | Daily mood check-ins | Free + premium |
| Sanvello | Digital CBT tools | Stress, anxiety self-care | CBT-based modules | Free + premium |
| Happify | Gamified mental wellness | Behavioral health skills | Activities & lessons | Subscription |
| Insight Timer | Meditation + support | Anxiety/stress management | Guided mindfulness | Free + premium |
| Calm | Meditation & sleep | Support for anxiety & insomnia | Meditation | Subscription |
| Headspace | Meditation + mental wellness | Stress & focus support | Meditation | Subscription |
Technological Innovations
Technology enhances therapy—but does not replace clinical judgment.
| Innovation | Function | Clinical Benefit | Risk |
| Secure Video Platforms | Live therapy | Remote access | Connectivity issues |
| EHR Systems | Documentation | Organized records | Privacy responsibility |
| AI Triage | Intake screening | Faster matching | Bias risk |
| Mood Tracking Apps | Daily logging | Measurement-based care | Over-tracking |
| Automated Scheduling | Efficiency | Reduced no-shows | Tech dependence |
| Digital CBT Modules | Guided exercises | Scalable treatment | Not for complex cases |
Products & Medication
Telehealth integrates medical treatment. Side effects mirror traditional prescribing and must be monitored professionally.
| Product Type | Purpose |
| SSRIs/SNRIs | Depression/anxiety management |
| Telepsychiatry Platforms | Medication oversight |
| Digital Journals | Behavioral tracking |
| Wearable Integration | Sleep/activity data |
Telehealth Counseling: Pros and Cons

Comparison with Other Mental Health Care Models
| Feature / Factor | Telehealth Counseling | Traditional In-Person Therapy | Mental Health Apps (Self-Guided) | Psychiatric Clinics / Hospitals | Community Counseling Centers |
| Primary Delivery Mode | Video, phone, chat | Face-to-face sessions | Mobile app modules | In-clinic evaluation & treatment | Local in-person services |
| Accessibility | High (location independent) | Limited by geography | Very high (24/7 app access) | Limited to facility location | Moderate (community-based) |
| Ideal For | Mild to moderate conditions | Moderate to severe cases needing rapport | Stress, mild anxiety, habit change | Severe mental illness, crisis care | Low-income or subsidized care |
| Crisis Handling | Limited (referral required) | Better immediate observation | Not suitable | Fully equipped for emergencies | Limited crisis capacity |
| Cost Structure | Subscription or per-session | Per-session billing | Monthly subscription | Insurance-based / high cost | Low-cost / sliding scale |
| Flexibility | High scheduling flexibility | Fixed appointments | On-demand self-paced | Fixed schedules | Appointment-based |
| Personalization | Moderate to high | High (direct therapist interaction) | Algorithm-driven | High clinical oversight | Moderate |
| Technology Dependence | High | Low | Very high | Moderate | Low |
| Privacy Considerations | Encrypted platforms required | Private office setting | Data stored digitally | Institutional protocols | Basic confidentiality standards |
| Therapist Interaction | Real-time but remote | Direct physical presence | None or minimal | Multidisciplinary team | Licensed counselors |
| Licensing Limitations | Cross-state restrictions | Local licensing | Not applicable | Hospital credentialing | Local licensing |
| Best Use Case Scenario | Remote professionals, rural patients | Deep trauma work, body-language cues needed | Preventive mental wellness | Acute psychiatric stabilization | Budget-sensitive ongoing therapy |
| Long-Term Sustainability | High (hybrid growth model) | Stable but resource-heavy | Scalable but limited depth | Essential for high-risk care | Community-dependent funding |
| Main Advantage | Convenience & scalability | Strong therapeutic alliance | Affordability & instant access | Intensive treatment capacity | Accessibility for underserved |
| Main Limitation | Limited for crisis/severe disorders | Travel & time constraints | Lacks human empathy | High cost & institutional setting | Limited specialist availability |
Global Telehealth Mental Health — Jobs, Salaries & Locations
| Job Title | Remote Possible | Primary Function | United States (Salary + Job Hubs) | United Kingdom (Salary + Job Hubs) | India (Salary + Job Hubs) | Australia / Canada (Salary + Job Hubs) | Middle East (UAE) (Salary + Job Hubs) |
| Telepsychiatrist | Yes | Diagnosis, medication management | $180K–$280K • New York, California, Texas (hospital networks, platforms like Teladoc Health) | $110K–$180K • London, Manchester (NHS + private) | $25K–$70K • Bengaluru, Hyderabad, Mumbai (private teleclinics) | $150K–$250K • Sydney, Toronto (public telehealth systems) | $160K–$260K • Dubai, Abu Dhabi (private hospitals) |
| Telehealth Psychologist | Yes | Therapy, assessments | $80K–$130K • California, Florida | $50K–$90K • London | $12K–$35K • Delhi, Chennai | $70K–$115K • Melbourne, Vancouver | $70K–$120K • Dubai |
| Licensed Therapist / Counselor | Yes | CBT, talk therapy | $60K–$100K • Nationwide remote | $40K–$65K • NHS regions | $8K–$25K • Metro cities | $60K–$95K • Urban centers | $55K–$95K • Private clinics |
| Clinical Social Worker (LCSW) | Yes | Therapy + case management | $60K–$95K • Chicago, Texas | $40K–$70K • Community trusts | $10K–$30K • NGOs, private setups | $60K–$90K • Provincial systems | $50K–$90K • Hospital networks |
| Care Coordinator (Telehealth) | Yes | Patient navigation, scheduling | $45K–$75K • Insurance companies | $30K–$55K • NHS admin | $6K–$18K • Private platforms | $45K–$70K • Public systems | $35K–$65K • Private providers |
| Clinical Director (Telehealth Platform) | Hybrid | Oversight, compliance | $90K–$150K • Large digital health firms | $70K–$130K • NHS/private mix | $20K–$60K • Growing startups | $100K–$160K • National health networks | $120K–$200K • Private hospital groups |
| Mental Health Coach (Non-clinical) | Yes | Behavioral support | $40K–$80K • App-based platforms | $30K–$55K • Private wellness | $5K–$20K • Startups | $40K–$75K • Employer wellness | $35K–$70K • Corporate programs |
Reviews
Avoid platforms without clear transparency. Before enrolling:
| Question | Why Important |
| Is the therapist licensed locally? | Legal compliance |
| What are cancellation policies? | Avoid fees |
| Is insurance accepted? | Cost control |
| What emergency protocol exists? | Safety |
| Are reviews verified? | Quality assurance |
FAQs
Is telehealth counseling effective?
For many mild-to-moderate conditions, yes. Severe crises often require hybrid care.
Can doctors prescribe medication online?
Yes, licensed psychiatrists can prescribe many medications subject to regulations.
Is it cheaper?
Often lower overhead reduces cost, but subscription structures vary.
Is it private?
Reputable platforms use encrypted systems compliant with medical regulations.
Who should avoid telehealth-only care?
Individuals experiencing acute psychiatric crises without local emergency support.
Final Perspective
Telehealth counseling is no longer an emergency substitute for in-person therapy—it is a structural redesign of how mental healthcare is delivered, accessed, and scaled. From rural patients connecting to licensed specialists across state lines to therapists building flexible, technology-enabled practices, the ecosystem now blends clinical expertise with digital infrastructure.
While challenges remain—regulatory complexity, privacy risks, and limitations in treating severe psychiatric conditions—the long-term trajectory points toward hybrid models that combine the relational depth of traditional care with the efficiency and reach of telemedicine.
The real opportunity lies not in replacing face-to-face therapy, but in expanding access, improving measurement, and creating sustainable mental health systems that work for both providers and patients.


