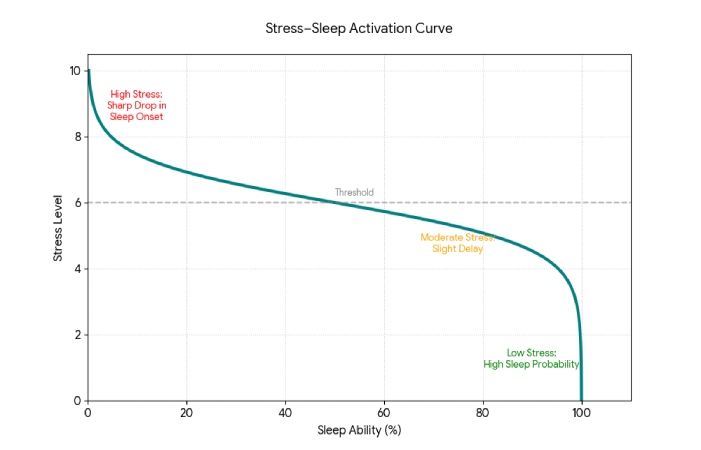
When you’re extremely stressed and can’t sleep, the problem isn’t a lack of sleep effort—it’s a nervous system stuck in threat mode. The fix is to lower arousal first, then let sleep happen as a side effect.
Most people try to “force” sleep—earlier bedtimes, melatonin, scrolling until exhaustion. That backfires. Stress activates cortisol and adrenaline, keeping your brain alert even when you’re exhausted. According to the American Academy of Sleep Medicine, chronic hyperarousal is a core driver of insomnia. Calm your body, contain your thoughts, optimize your environment, and—if needed—use structured therapy like CBT-I.
Overview: Stress, Anxiety & Sleep
Stress activates the hypothalamic-pituitary-adrenal (HPA) axis. Cortisol rises. Heart rate increases. Muscles tighten. That’s adaptive for danger—but incompatible with deep sleep. The National Institutes of Health notes that persistent sleep disruption increases risks of anxiety, depression, metabolic disease, and impaired immunity.
| Aspect | Explanation |
| Core Problem | Nervous system hyperarousal |
| Common Trigger | Work pressure, exams, financial stress, health anxiety |
| Hormonal Driver | Cortisol + adrenaline |
| Sleep Stage Impact | Reduced REM + fragmented deep sleep |
| Short-Term vs Chronic | Acute (days–weeks) vs conditioned insomnia (months) |
| Evidence Base | Behavioral therapy preferred over sedatives |
Sleep Anxiety Symptoms
| Symptom | What It Feels Like | Why It Happens |
| Racing thoughts | Mind won’t “switch off” | Cognitive hyperarousal |
| Fast heartbeat | Chest pounding | Sympathetic activation |
| Muscle tension | Jaw/shoulder tightness | Fight-or-flight |
| Clock watching | Repeated time checking | Performance anxiety |
| Early waking | 3–5 a.m. alertness | Cortisol spike |
If these occur most nights for 2+ weeks, structured intervention is recommended.
Stress Type vs Sleep Pattern
| Stress Type | Body Reaction | Sleep Pattern |
| Work deadline | Elevated evening cortisol | Delayed sleep onset |
| Emotional conflict | Increased heart rate | Restless sleep |
| Anticipatory anxiety | Hypervigilance | Early morning awakening |
| Chronic overload | Sustained arousal | Fragmented REM |
Immediate Relaxation Techniques (5–15 Minutes)
| Technique | How to Do It | Duration | Best For |
| 4-7-8 Breathing | Inhale 4s, hold 7s, exhale 8s | 4 cycles | Rapid calming |
| Progressive Muscle Relaxation | Tense & release muscles | 10 mins | Body tension |
| Box Breathing | 4-4-4-4 pattern | 5 mins | Panic spikes |
| Body Scan | Focus attention body-part by body-part | 10 mins | Rumination |
| Cold splash + slow breath | Cold face + exhale | 2 mins | Acute anxiety |
Mental Unloading Strategies
| Strategy | When to Use | Why It Works |
| Worry Window (scheduled earlier) | Evening | Contains anxiety |
| Brain Dump Journal | Before bed | Externalizes rumination |
| “Tomorrow List” | 1–2 hrs pre-sleep | Reduces task anxiety |
| Cognitive Shuffle | In bed | Distracts analytical brain |
What Is the 10-3-2-1-0 Rule?
| Number | Rule | Why |
| 10 | No caffeine 10 hrs before bed | Caffeine half-life |
| 3 | No heavy meals/alcohol 3 hrs before | Digestion disrupts sleep |
| 2 | No work 2 hrs before | Cortisol reduction |
| 1 | No screens 1 hr before | Blue light suppression |
| 0 | 0 snooze button | Stabilizes rhythm |
The Centers for Disease Control and Prevention emphasizes consistent sleep schedules as foundational for circadian regulation.
Supplement Reality Check
| Supplement | Evidence Level | Use Case |
| Melatonin | Moderate | Jet lag, circadian shift |
| Magnesium glycinate | Limited–Moderate | Muscle tension |
| L-theanine | Emerging | Mild anxiety |
| Ashwagandha | Mixed | Chronic stress |
None override poor stress regulation habits
How to Calm Anxiety to Sleep
Lower body arousal (breathing).

When to Seek Professional Help
Consult a clinician if:
- Insomnia lasts >3 months
- Nighttime panic attacks occur
- Severe depression or anxiety symptoms
- Snoring + gasping (possible sleep apnea)
- Reliance on alcohol or pills
Chronic insomnia is a treatable medical condition.
What Are the Treatments Available?
| Treatment | Availability | Effectiveness | Risk |
| CBT-I | US, UK, India, EU, Australia | High | Low |
| Sleep Medications | Global | Moderate | Dependency risk |
| Melatonin | OTC in many countries | Mild–Moderate | Low |
| Digital CBT-I Apps | Global | Moderate–High | Low |
| Sleep Clinics | Urban centers worldwide | High | Cost |
Services Available in Sleep Clinics
| Service | Purpose |
| Polysomnography | Diagnose sleep apnea |
| CBT-I Sessions | Treat insomnia |
| Anxiety Counseling | Stress management |
| Medication Review | Optimize prescriptions |
| Circadian Rhythm Testing | Identify delayed sleep phase |
Medical Tests
| Department | Tests |
| Pulmonology | Sleep apnea study |
| Neurology | Narcolepsy evaluation |
| Psychiatry | Anxiety disorder screening |
| ENT | Airway obstruction |
| Endocrinology | Thyroid panel |
Specialists & Qualifications
| Specialist | Qualification | Focus |
| Sleep Physician | MD + Sleep Fellowship | Diagnosis |
| Clinical Psychologist | MPhil/PhD | CBT-I |
| Psychiatrist | MD Psychiatry | Medication |
| Respiratory Therapist | Certified Technician | Sleep studies |
Doctors Fees
| Country | Consultation Fee | CBT-I Package | Sleep Study Cost |
| US | $150–300 | $800–1500 | $1000–3000 |
| UK | £100–250 | £600–1200 | £800–2000 |
| India | ₹800–2500 | ₹10,000–25,000 | ₹8,000–20,000 |
| Australia | AUD 150–300 | AUD 700–1400 | AUD 1000–2500 |
Insurance Details
| Coverage Type | Usually Covered? |
| Sleep Study | Yes (with referral) |
| CBT-I | Sometimes |
| Medication | Yes |
| Apps | No |
Locations
| Region | Major Cities |
| North America | New York, Toronto |
| Europe | London, Berlin |
| Asia | Mumbai, Singapore |
| Australia | Sydney, Melbourne |
Tools & Apps
| Tool/App | Type | Use |
| Headspace | Meditation App | Guided sleep |
| Calm | Meditation App | Sleep stories |
| Oura Health | Wearable | Sleep tracking |
| Philips CPAP | Device | Apnea |
Always confirm pre-authorization requirements.
Pros and Cons of Common Sleep Solutions
Alcohol may induce drowsiness but disrupts REM sleep and increases awakenings. Medications work quickly but risk tolerance and dependency. Supplements like melatonin help circadian timing but not stress arousal. Relaxation techniques are safe and build resilience, but require practice. CBT-I takes weeks but produces durable change. Faster solutions offer immediate relief; structured behavioral therapy offers lasting correction.
Pros
- Helpful for circadian shift
- Fast sedation
- Strong short-term
- Long-term solution
- Stress reduction
Cons
- Not strong for stress insomnia
- REM disruption
- Dependency risk
- Requires effort
- Takes time
At-Home vs Professional Solutions
| Factor | At-Home Methods | Professional Treatment |
| Cost | Low | Moderate |
| Speed | Variable | Structured |
| Sustainability | Medium | High |
| Personalization | Low | High |
| Insurance | Not applicable | Often covered |
Reviews
| Solution | User Feedback Trend |
| CBT-I | High satisfaction long-term |
| Meditation Apps | Good short-term calm |
| Sleeping Pills | Effective but dependency concerns |
| Wearables | Useful awareness |
FAQs
How to sleep when extremely stressed?
Lower arousal first (breathing), unload thoughts (journaling), then optimize the environment.
How to calm anxiety to sleep?
Slow breathing + cognitive shuffle + consistent bedtime routine.
What is the 10-3-2-1-0 Rule?
A structured wind-down system reducing caffeine, food, work, screens, and snoozing.
When to see a doctor?
If symptoms persist beyond 2–4 weeks or include severe anxiety/depression.
Final Perspective
Stress-driven sleep problems are not a sign of weakness or failure—they are a predictable biological response to perceived threat. The solution is not to control sleep, but to reduce arousal. When you calm the body, contain the mind, and remove performance pressure, sleep becomes a byproduct rather than a goal.
For short-term stress, simple regulation tools are often enough. For persistent insomnia, structured approaches like CBT-I—endorsed by the American Academy of Sleep Medicine—offer durable results. The shift is simple but powerful: stop chasing sleep and start creating safety.