The keyword “apothorax in human body” is commonly used in search results, but in medical science the correct term is pneumothorax (collapsed lung). For clarity, this guide will use apothorax in human body while explaining the clinically accurate concept.
In India, this condition carries distinct epidemiological patterns due to high tuberculosis (TB) burden, rising air pollution, occupational exposure, and trauma incidence. Unlike Western countries, where smoking-related lung disease dominates, India presents a mixed-risk profile—making localized understanding essential for both patients and healthcare professionals.
What Is Apothorax in Human Body?
Apothorax in human body refers to a condition where air accumulates in the pleural cavity, the space between the lung and chest wall. This disrupts the negative pressure required to keep the lungs inflated, leading to partial or complete lung collapse.
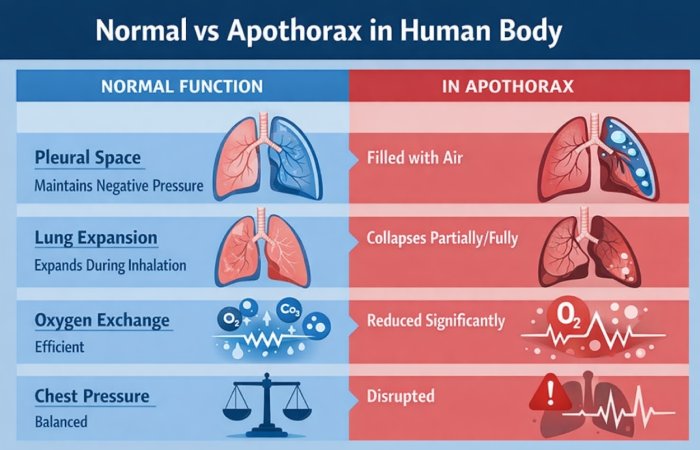
In Indian clinical settings, especially in government hospitals, patients often present late-stage collapse, not because of disease severity but due to delayed diagnosis and awareness gaps.
Types of Apothorax in Human Body
Understanding the types is crucial because treatment decisions vary significantly.
| Type | Definition | Common in India? | Key Risk Group |
| Primary Spontaneous | No underlying disease | Moderate | Young smokers |
| Secondary Spontaneous | Due to lung disease | Very High | TB and COPD patients |
| Traumatic | Injury-related | High | Accident victims |
| Iatrogenic | Medical procedure-related | Increasing | Hospital patients |
| Tension Apothorax | Severe, life-threatening | Critical cases | ICU/emergency |
1. Primary Spontaneous Apothorax
Occurs without any known lung disease. Increasing urban smoking habits are contributing to a rise in cases among young adults.
| Factor | Explanation |
| Body Type | Tall, thin individuals are more prone |
| Smoking | Major trigger |
| Age Group | 15–35 years |
2. Secondary Spontaneous Apothorax
| Cause | India-Specific Importance |
| Tuberculosis (TB) | Leading cause |
| COPD | Due to smoking + biomass fuel |
| Lung infections | Common in rural populations |
India accounts for a significant share of global TB cases, making TB-induced apothorax one of the most important differentiators from Western epidemiology.
3. Traumatic Apothorax
| Cause | Indian Context |
| Road accidents | Very high incidence |
| Falls | Construction workers at risk |
| Assault injuries | Urban trauma centers |
4. Iatrogenic Apothorax
| Procedure | Risk Level |
| Central line insertion | Moderate |
| Lung biopsy | Moderate |
| Ventilation | High in ICU |
Rising due to increased medical procedures and ICU care expansion in India.
5. Tension Apothorax (Emergency)
| Feature | Impact |
| Air trapping | Rapid pressure buildup |
| Heart displacement | Circulatory collapse |
| Oxygen drop | Life-threatening |
Cost Analysis in India
| Procedure | Cost Range (INR) |
| X-ray | ₹300 – ₹800 |
| CT Scan | ₹2,000 – ₹5,000 |
| Chest Tube | ₹10,000 – ₹40,000 |
| Surgery | ₹1.5 – ₹3 lakh |
Doctor Types and Their Roles
| Doctor Type | Role in Treatment | When You Need Them | Availability in India |
| Pulmonologist | Diagnoses and manages lung conditions | First consultation, mild to moderate cases | Widely available in urban areas |
| Thoracic Surgeon | Performs surgical interventions (VATS, pleurodesis) | Severe or recurrent cases | Available in tertiary hospitals |
| Emergency Medicine Doctor | Handles acute and life-threatening cases | Sudden collapse, trauma, tension cases | Present in most hospitals |
| General Physician | Initial diagnosis and referral | Early symptoms or confusion with other conditions | Available everywhere |
| Critical Care Specialist | Manages ICU patients | Severe respiratory distress | Available in major hospitals |
Top Doctors for Apothorax in Human Body Treatment – With Fees
Pulmonologists and thoracic specialists relevant for treating apothorax in human body.
| Doctor Name | Specialty | Hospital / Practice | City | Experience | Consultation Fee (INR) |
| Dr. Jagdish Chander Suri | Pulmonologist | Fortis Hospital | New Delhi | 35+ years | ₹2000 |
| Dr. Arun Sampath | Pulmonologist | MIOT International | Chennai | 20+ years | ₹800 |
| Dr. Ayush Gupta | Pulmonologist | Fortis Hospital | New Delhi | 15+ years | ₹1200 |
| Dr. Puneet Khanna | Pulmonologist | Manipal Hospital | Delhi | 20+ years | ₹1100 |
| Dr. Ammaiyappan Palaniswamy Chockalingam | Pulmonologist | MGM Healthcare | Chennai | 25+ years | ₹800 |
| Dr. Abhinav Guliani | Pulmonologist | Sir Ganga Ram Hospital | New Delhi | 15+ years | ₹1500 |
| Dr. Manjunath B G | Pulmonologist | Medicover Hospitals | Bangalore | 15+ years | ₹600 |
| Dr. Huliraj N | Pulmonologist | Vydehi Hospital | Bangalore | 30+ years | ₹800–₹1500 |
| Dr. Pankul Mangla | Pulmonologist | Private Practice | Delhi | 10+ years | ₹1200 |
| Dr. Nipun Agrawal | Pulmonologist | Private Practice | Madhya Pradesh | 8+ years | ₹500 |
Hospitals for Apothorax Treatment in India
| Hospital Name | City | Type | Key Specialty for Apothorax | Facilities Available | Approx Cost Level |
| All India Institute of Medical Sciences (AIIMS) | New Delhi | Government | Pulmonology, Thoracic Surgery | ICU, CT Scan, Chest Tube, VATS | Low |
| Apollo Hospitals | Chennai | Private | Advanced Lung Care | ICU, Robotic Surgery, Emergency Care | High |
| Medanta – The Medicity | Gurugram | Private | Thoracic Surgery | VATS, ICU, Advanced Imaging | High |
| KIMS Hospitals | Hyderabad | Private | Emergency & Critical Care | ICU, Trauma Care, Chest Tube | Moderate–High |
| Tata Memorial Hospital | Mumbai | Government | Pulmonary & Chest Diseases | Imaging, ICU, Surgical Care | Low |
| Fortis Hospital | Bangalore | Private | Respiratory Medicine | ICU, CT Scan, Emergency | High |
| Max Super Specialty Hospital | New Delhi | Private | Pulmonology & Surgery | ICU, VATS, Advanced Diagnostics | High |
| Narayana Health | Bangalore | Private | Affordable Critical Care | ICU, Surgery, Imaging | Moderate |
| PGIMER | Chandigarh | Government | Advanced Pulmonology | ICU, CT Scan, Emergency | Low |
| Osmania General Hospital | Hyderabad | Government | Emergency & Chest Care | Basic ICU, X-ray, Chest Tube | Very Low |
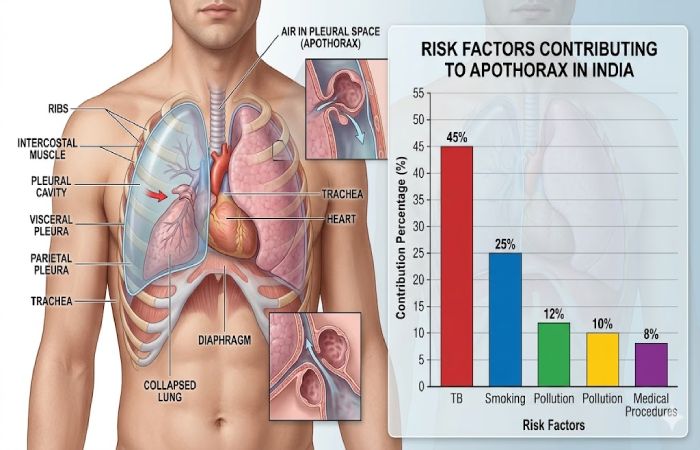
Causes of Apothorax in India
| Category | Cause | Relative Impact |
| Infectious | Tuberculosis | Very High |
| Environmental | Air Pollution (PM2.5) | High |
| Lifestyle | Smoking | High |
| Occupational | Dust, chemicals | Moderate |
| Trauma | Accidents | High |
| Medical | Procedures | Growing |
India’s dual burden of infectious disease (TB) and environmental exposure creates a unique overlap, increasing vulnerability even in non-smokers.
Symptoms of Apothorax in Human Body
| Symptom | Description | Severity Indicator |
| Chest Pain | Sharp, sudden | Early sign |
| Breathlessness | Difficulty breathing | Moderate |
| Rapid Pulse | Increased heart rate | Stress response |
| Fatigue | Low oxygen levels | Mild–moderate |
| Cyanosis | Blue lips/skin | Severe |
| Confusion | Oxygen deprivation | Emergency |
Patients often confuse symptoms with:
- Gas/acidity
- Muscle strain
- Mild respiratory infection
This leads to delayed hospital visits and worsening outcomes.
Diagnosis in India
Diagnostic Methods
| Method | Purpose | Availability |
| Chest X-ray | First-line detection | Widely available |
| CT Scan | Detailed imaging | Urban hospitals |
| Ultrasound | Emergency detection | Increasing |
| ABG Test | Oxygen measurement | Tertiary centers |
Urban vs Rural Gap
| Factor | Urban India | Rural India |
| Diagnostic Speed | Fast | Slower |
| Technology Access | Advanced | Limited |
| Specialist Availability | High | Low |
Treatment Options in India
| Treatment | When Used | Outcome |
| Observation | Small cases | Self-healing |
| Oxygen Therapy | Mild cases | Faster recovery |
| Needle Aspiration | Moderate cases | Air removal |
| Chest Tube (ICD) | Severe cases | Standard treatment |
| Surgery (VATS) | Recurrent cases | Prevent recurrence |
Recovery and Prognosis
Recovery Timeline
| Case Type | Duration |
| Mild | 1–2 weeks |
| Moderate | 2–4 weeks |
| Severe | 4–6 weeks |
| Post-Surgery | 6–8 weeks |
Recurrence Risk
| Risk Factor | Recurrence Chance |
| Smoking | High |
| TB history | Very High |
| No treatment | Extremely High |
Complications
| Complication | Impact |
| Recurrence | Common |
| Infection | Hospital risk |
| Lung damage | Long-term |
| Respiratory failure | Severe cases |
Prevention Strategies
| Strategy | Practical Application |
| Quit smoking | Reduces primary risk |
| TB control | Early diagnosis & treatment |
| Pollution protection | Masks, air purifiers |
| Workplace safety | PPE in high-risk jobs |
| Regular checkups | High-risk individuals |
India vs Global Comparison
| Factor | India | Western Countries |
| Leading Cause | Tuberculosis | Smoking |
| Awareness | Low | Moderate |
| Diagnosis Delay | High | Low |
| Healthcare Access | Uneven | Better |
Expert Reviews
Most global treat this condition as a purely respiratory emergency, but in India, it functions as a system-level indicator of:
- Underlying cause is critical: Experts highlight that apothorax (pneumothorax) is often a sign of hidden lung disease, not just a standalone condition, requiring deeper investigation.
- CT scan is the gold standard: While X-rays are commonly used, specialists emphasize that CT imaging provides more accurate diagnosis and cause identification, especially in complex cases.
- TB is a major driver in India: Indian studies consistently show that tuberculosis is one of the leading causes, unlike Western countries where smoking dominates.
- Conservative treatment is evolving: Recent research suggests that observation and oxygen therapy can be effective in stable cases, reducing complications and hospital stay.
- High recurrence risk: Experts warn that recurrence is common, especially if underlying conditions like TB or COPD are not treated properly.
FAQs
Is apothorax in human body dangerous?
Yes, especially severe forms can be life-threatening if untreated.
Can it heal without treatment?
Small cases may heal, but medical supervision is necessary.
Why is it more common in India?
Due to TB, pollution, and trauma rates.
Can it happen again?
Yes, recurrence is common without proper management.
Conclusion
Apothorax in human body is a serious yet treatable condition, but its Indian context changes everything. The dominance of tuberculosis, rising pollution, and uneven healthcare access make early detection and prevention critical. A shift toward awareness, early diagnosis, and integrated public health strategies can significantly reduce its burden.